Manual Therapy is a broad term used to describe a multitude of approaches and techniques where the clinician uses their hands to effect change in soft tissues and joints. The aim is generally to improve and/or restore mobility and motion.
The techniques and approaches vary considerably and clinicians often pursue a specialization to obtain mastery of a particular technique.
Manual therapy is well liked by clinicians and patients because of the hands-on nature of the interventions. Its effect has been demonstrated in many conditions, including low back pain, neck pain, disc degeneration, trigger points, and many others.
Manipulation, Adjustment, Mobilization?
Many people think of bone-popping, joint-cracking thrust maneuvers when they think of manual therapy. While these maneuvers are definitely part of the manual therapy arsenal, they are but a small part of it. The therapist could be using very gentle manual pressure to coax a muscle into relaxation or apply stronger pressure to stretch some stiff tissue after a joint has been immobilized for a while.
The following are some specific techniques that are performed at this clinic.
Spinal Decompression
Decompression is an approach aiming to decrease or relieve pressure inside a intervertebral disc in the spine.
When a disc gets injured, it may start bulging to the outside, which can then put pressure on the surrounding tissues. This will cause pain, muscle tension or spasm, nerve pain and possibly symptoms radiating into the arm or leg. Therapy aims to encourage the disc to reabsorb the bulging nucleus but it is often hard to do. Decompression helps.
With decompression the therapist applies traction to the lower part of the spine while the upper part of the spine is fixed to the table. In other words, the spine is being pulled apart a little. This causes a decrease of pressure on the inside of the bulging disc, thus helping the disc to heal.
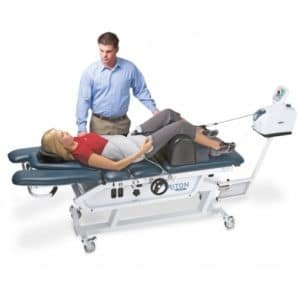
The approach is best performed when the manual intervention is assisted by advanced mechanical traction devices. These devices mimic the hands of therapist, gradually applying traction and then releasing it, repeating that multiple times over a period of 30 minutes or so. The advantage of using mechanical devices to complement the manual intervention is the precision and reliability of the traction. The device can be programmed to deliver exactly what the patient needs for exactly the right amount of time and do so reliably and consistently every single time.
Limitations
While Manual Therapy is used for many conditions treated here, it is almost never the only treatment intervention. Others may include exercise, postural correction, advanced therapeutic modalities such as shockwave, magnetic stimulation and biofeedback.
The skillful combination of these interventions is what makes the overall therapy so effective.
References
Ajimsha, M. S. "Effectiveness of direct vs indirect technique myofascial release in the management of tension-type headache." Journal of bodywork and movement therapies15.4 (2011): 431-435.
Fredin, Ken, and Håvard Lorås. "Manual therapy, exercise therapy or combined treatment in the management of adult neck pain–A systematic review and meta-analysis." Musculoskeletal Science and Practice 31 (2017): 62-71.
Ghodrati, Maryam, et al. "The Effect of Combination Therapy; Manual Therapy and Exercise, in Patients With Non-Specific Chronic Neck Pain: A Randomized Clinical Trial." Physical Treatments-Specific Physical Therapy Journal 7.2 (2017): 0-0.
Yaseen, Khalid, et al. "The effectiveness of manual therapy in treating cervicogenic dizziness: a systematic review." Journal of physical therapy science 30.1 (2018): 96-102.